A new, excellent and useful resource – a report published by British Psychological Society, Division of Clinical Psychology.
It’s available as a free pdf download – see the links below.
 “One of the most important messages of this report is that there is no dividing line between ‘psychosis’ and ‘normality’.”
“One of the most important messages of this report is that there is no dividing line between ‘psychosis’ and ‘normality’.”
“A fundamental message of this report is that ‘psychotic’ experiences are understandable in the same ways as ‘normal’ experiences, and can be approached in the same way.”
Selected Key Messages …
Key Messages those working in Mental Health Services
- Professionals need to be open about the fact that prescribing is pragmatic: finding out whether medication is likely to help someone, and if so which drug and dose, is always a trial-and-error process.
- In particular, professionals should not insist that people agree with the view experiences are symptoms of an underlying illness.
- Professionals need to acknowledge that the only way someone can find out for sure what helps them personally is to try things out.
- Lived experience of mental health problems should be recognised as an important source of knowledge alongside ‘book-learning’ for professionals.
- Our role is to provide information about what is available and what others have found helpful, and then support people to choose.
- Services should see personal experience of mental health problems as ‘desirable’ in their selection criteria for staff, including senior clinicians.
- Training by people with personal experience is vital, both with regard to how people understand their difficulties, and also with regard to what helps and what doesn’t.
Key Messages for all of us
- If we are serious about preventing distressing ‘psychosis’ we need to tackle deprivation, abuse and inequality.
- There is no ‘us’ and ‘them’ – we’re all in this together. Many of us hear voices occasionally, or have fears or beliefs that those around us do not share. Given enough stress, for any of us these experiences might shade into psychosis.
- This report has highlighted the complex causes of distressing psychotic experiences.What is encouraging is that many of the causes are things that we can do something about.
- There is a parallel here with public health in the physical arena, namely that some of the steps that need to be taken are economic, social and even political.
- Evidence shows that a major contribution to serious emotional distress is not only poverty but particularly income inequality – the growing gap between the richest and poorest people in society.
- There is no doubt that people who have been subject to oppression, and particularly discrimination (racism, homophobia, discrimination on grounds or gender, disability or ‘mental health’) are put at risk by these experiences.
- We need to campaign against prejudice and discrimination on ‘mental health’ grounds.
________________________________________________________
Part four of the report sets out what we need to do differently, and is divided into are two sections.:
13 What Mental Health services need to do differently.
14 What we all need to do differently.
Part 4 What We Need To Do Differently
Section 13 What Mental Health Services Need to Do Differently
13.1 We need to move beyond the “medical model”
13.2 We need to replace paternalism with collaboration
13.2.1 Listening
Professionals often underestimate the power of simply listening. Careful listening is an essential prerequisite of offering appropriate help, and it is also a powerful form of help in its own right. Many people say that lack of listening is what most disappoints them about services.
13.2.2 Accepting views other than the medical model Some people view their difficulties as a medical illness, some see them as a reaction to things that have happened in their life, some as spiritual experiences, and others as a combination of these.
In the past, rejection of an illness view has sometimes been seen as ‘lack of insight’, sometimes even as ‘part of the illness’. However, it is unhelpful to insist that people accept any one particular framework of understanding.
In particular, professionals should not insist that people agree with the view that experiences are symptoms of an underlying illness. Some people will find this a useful way of thinking about their difficulties and others will not.
13.2.3 Collaboration rather than just ‘involvement’ Professionals must listen to what service users and former service users have to say about services and treatments – it is only by listening that we can learn what really is helpful.
It should be standard practice for service users to be involved at all levels, from planning the service as a whole to providing feedback to individual teams and, perhaps most importantly, in planning their own care.
Lived experience of mental health problems should be recognised as an important source of knowledge alongside ‘book-learning’ for professionals.
As some NHS Trusts already do, services should see personal experience of mental health problems as ‘desirable’ in their selection criteria for staff, including senior clinicians.
13.3 We need to stop telling people what to do and start supporting them to choose
13.3.1 Trying Things Out
Professionals need to acknowledge that the only way someone can find out for sure what helps them personally is to try things out. Our role is to provide information about what is available and what others have found helpful, and then support people to choose.
13.3.2 Talking therapy It remains scandalous that despite the NICE recommendations, still only a minority of people are offered talking therapy. Psychological help should be available to all, as should help for family members who support people experiencing psychosis.
13.3.3 Medication or no medication Service users and their supporters have the right to information about the pros, cons, possible adverse effects (‘side-effects’) and evidence base for any medication that is offered.
Particularly when contemplating taking medication long-term, people should be encouraged and supported to ask questions about the drugs and any alternatives.
Professionals need to be open about the fact that prescribing is pragmatic: finding out whether medication is likely to help someone, and if so which drug and dose, is always a trial-and-error process.
We also need to provide information about the best way to come off medication if that is what the person wants to do, and to support them in the process.
13.3.4 Professional help, peer support or self-help As we explained above, many people will prefer community-based or self-help approaches to any kind of professional treatment. Professionals need to give people information about groups affiliated to organisations such as Mind, Bipolar UK, Rethink Mental Illness, Together, Intervoice, the Hearing Voices Network and the Paranoia Network.
13.4 We need to make rights and expectations explicit As any treatment has the potential to do harm as well as good, the principle of informed consent is paramount. People should have the right to refuse treatments, from ECT to medication and psychological therapies.
13.5 We need to reduce the use of compulsion and mental health legislation
13.5.1 Changing the culture of psychiatric hospitals Mental health wards can be aversive places to be, particularly for anyone who does not think of difficulties as an illness. This is probably the main reason that mental health legislation has to be invoked so frequently to keep people in hospital. We need to create places that people want to go to when they are in a crisis, where care is informed by the approach outlined in this report. Acute wards need to change so that they operate on the principles outlined here. Every district should also have at least one non-medical crisis house.
13.5.2 Is mental health legislation inherently discriminatory? Many psychologists feel that the existence of separate legislation which applies only to people deemed ‘mentally ill’ is discriminatory, particularly in view of the problems we have outlined with the whole idea of ‘mental illness’.
13.5.3 Is forced medication ever justified? Some psychologists take the view that whilst compulsory detention can sometimes be justified in order to keep someone safe, it becoming increasingly hard to justify forced medication.
The United Nations Special Rapporteur on Torture and Other Cruel, Inhuman or Degrading Treatment has called for a ban20 on forced psychiatric treatment including drugging, ECT (electro-convulsive therapy), psychosurgery, restraint and seclusion.
13.6 We need to change the way we do research Firstly, research efforts have been weighted too heavily towards the search for biological abnormalities. The focus of research needs to turn much more towards the events and circumstances of people’s lives, and the way that these affect us at a social, psychological and even biological level.
The issue of funding for research is also important. Traditionally, drug companies have funded much medical research into ‘schizophrenia’. This raises several important issues. Firstly, this research has often been based on the assumption that the tendency to experience psychosis is primarily a biological phenomenon. As this report has demonstrated, both this assumption and also the view that everyone who has a diagnosis of schizophrenia needs to take medication, are increasingly being challenged.
A second issue surrounding drug company funding is one of reliability and bias of findings. Concerns that studies funded by drug companies selectively publish positive findings, and do not publish negative results, have been supported by a number of studies.
The profound effects of the pharmaceutical industry’s vested interests have been summarised in a paper called Drug companies and schizophrenia: Unbridled capitalism meets madness. There remains an urgent need for more research funding that is independent of drug companies, and for research which focuses on psychological, social and self-help approaches.
13.7 We need to change how mental health professionals are trained and supported Perhaps even more important than the availability of specific talking treatments is the need for all mental health workers to be aware of the information contained in this report. Many workers are unaware of the psychological perspective on psychosis, and are unfamiliar with the research described in this report.
A fundamental message of this report is that ‘psychotic’ experiences are understandable in the same ways as ‘normal’ experiences, and can be approached in the same way.
This message needs to form the core of pre- and post-qualification training. A manual for a two-day training course is available, Psychosis Revisited, based on our earlier report and designed to be delivered by a professional in collaboration with someone who has themselves experienced psychosis.
Training by people with personal experience is vital, both with regard to how people understand their difficulties, and also with regard to what helps and what doesn’t.
The Health and Care Professions Council has recently made service user involvement mandatory in professional training courses.
Counsellors and therapists working in primary care or in secondary care psychological services often lack training in working with people who experience psychosis – indeed, often such services specifically exclude people who have experienced psychosis. This needs to change.
These changes need not be expensive. We are suggesting a change in the way that all professionals are trained and approach their work, rather than necessarily recruiting many additional staff. Training costs money, but we are already paying for training, and it needs to change to reflect our developing understanding of the nature of psychosis. What we are recommending is more fundamental than increased resources: a change in the guiding idea behind services.
Finally, staff can only offer the compassion and emotional support that people need when they are themselves supported and shown compassion by their organisation, and when the demands on them are reasonable. It is vital that rather than being quick to criticise, we recognise how demanding mental health work can be and also acknowledge its vital importance in our society.
Section 14: What we all need to do differently
Key points There is no ‘us and them’, people who are ‘normal’ and people who are different because they are ‘mentally ill’. We’re all in this together and we need to take care of each other.If we are serious about preventing distressing ‘psychosis’ we need to tackle deprivation, abuse and inequality.
14.1 We need take on board that we’re all in this together – there is no ‘us’ and ‘them’
One of the most important messages of this report is that there is no dividing line between ‘psychosis’ and ‘normality’.
There is no ‘us’ and ‘them’ – we’re all in this together. Many of us hear voices occasionally, or have fears or beliefs that those around us do not share. Given enough stress, for any of us these experiences might shade into psychosis.
Sometimes what constitutes ‘psychosis’ is in the eye of the beholder: for example, if someone does not get on with his or her neighbours, is frightened of them and suspects their involvement when things go wrong, when does this shade into ‘paranoia’?
The main way that we all need to change is by taking on board that there is no ‘us’ and ‘them’, there are only people trying to make the best of our situation.
14.2 We need to focus on prevention
This report has highlighted the complex causes of distressing psychotic experiences.What is encouraging is that many of the causes are things that we can do something about.
There is a parallel here with public health in the physical arena, namely that some of the steps that need to be taken are economic, social and even political.
A famous example of the huge difference that public health measures can make is that of Dr William Duncan in nineteenth century Liverpool. As with most doctors in Victorian Britain, Duncan came from a privileged background. But after working as a GP in a working-class area of Liverpool, he became interested in the links between poverty and ill-health and started researching the living conditions of his patients. He was shocked by the poverty he found, and in the clear link between housing conditions and the outbreak of diseases such as cholera, smallpox and typhus. He started a lifelong campaign for improved living conditions, particularly better housing, cleaner water and better drains, which led to huge improvements in the health of many thousands of people.
So what might be the mental health equivalent of clean water and sanitation?
The evidence suggests that two things are particularly important: safety and equality. These are addressed in the following paragraphs, together with other issues that we need to tackle in order to reduce the rates of mental health problems in our society.
14.2.1 Prevention: Safety
To feel safe and secure we need to know that our basic needs will be met. This is why efforts to reduce poverty, and particularly child poverty, are so important if we are to reduce the numbers of people who go on to experience distressing psychosis.
To feel safe and secure we also need to be able to trust those in positions of power over us. In particular, when we are growing up we need to be able to trust the adults who are entrusted with our care. This is why efforts to reduce child abuse and neglect are central to efforts at preventing psychosis as well as other mental health problems. We all need to work with teachers, social workers, community nurses, GPs and the police to identify and then respond to early warning signs that children might be exposed to sexual, physical or emotional abuse, neglect or bullying. As parents we need to seek support ourselves if we worry that our own stress is having an impact on our children.
Children who have been exposed to these things need support and nurturing and there is evidence that where this happens, the likelihood of hearing distressing voices later in life, for example, is much reduced.
14.2.2 Prevention: Equality
Evidence shows that a major contribution to serious emotional distress is not only poverty but particularly income inequality – the growing gap between the richest and poorest people in society.
In their book The Spirit Level, sociologists Richard Wilkinson and Kate Pickett demonstrate that mental health problems are highest in those countries with the greatest gaps between rich and poor, and lowest in countries with smaller differences. Equal societies are associated with more trust and less paranoia.
This suggests that rather than primarily targeting our efforts at individuals, the most effective way to reduce rates of ‘psychosis’ might be to reduce inequality in society.
14.2.3 Prevention: Reducing discrimination and oppression
A classic paper published in 1994 was entitled Environmental failure – Oppression is the only cause of psychopathology. Whilst some might think that goes too far, there is no doubt that people who have been subject to oppression, and particularly discrimination (racism, homophobia, discrimination on grounds or gender, disability or ‘mental health’) are put at risk by these experiences.
We can all work to combat discrimination and promote a more tolerant and accepting society.
14.2.4 Prevention: Reducing harmful drug use and addressing its causes
Alcohol is unquestionably the most serious substance-related public health issue, but cannabis and other drugs have been associated with mental health problems in general and psychosis in particular. Over-use of recreational drugs appears to make it more likely that someone will experience a psychotic crisis. This does not necessarily mean that we need a stronger clamp-down on drugs – the so-called ‘war on drugs’ does not appear to have been won, and many people argue that de-criminalising the possession and use of drugs would be an important positive step towards protecting people’s health. It is also important to address the social problems that lead people to turn to taking drugs, including poverty, inequality, unemployment, hopelessness and feeling disenfranchised from society.
14.2.5 Prevention: What we can each do to protect our mental health
So far, this section has concentrated on what we can do together to reduce the risk that some of us will experience distressing ‘psychosis’.
However, research also suggests that there are things that we can each do ourselves to protect our own mental health.
Firstly, we can look after ourselves physically: as we saw above, getting regular, good sleep is vitally important, as are nutritious food, exercise, and exposure to open air and green spaces. We can exercise caution with recreational drugs, even very commonplace drugs such as alcohol or cannabis.
Since our social environment is also vital, we can usefully examine our relationships with family, friends and colleagues and take steps to resolve sources of stress.
Money worries are one of the most common stressors. Although our income is often beyond our control, we can take steps to deal with debt, to plan for retirement, to manage our finances, and to plan for the future (psychologists call this ‘adaptive coping’).
Finally, we all experience major negative events during our lives, such as when someone close to us dies. Whilst we can’t prevent things happening, we have some control over how we respond. For example, do we tend to jump to conclusions or take things personally? Sometimes it can help to talk over with a friend or counsellor how and why we habitually respond the way we do, and any changes we could make.
The New Economics Foundation’s ‘Five Ways to Wellbeing’ framework might be of use here.
14.3 We need to campaign against prejudice and discrimination on ‘mental health’ grounds
This report has shown how we can be affected as much by the reaction of people around us as by the actual experiences themselves.
For example, people who are seen as ‘mentally ill’ often experience prejudice, rejection and social exclusion, which can be significant – sometimes even insurmountable – obstacles to recovery.
For many people, prejudice based on misinformation presents a greater obstacle than the original mental health problems.
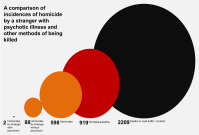
Too many people have been taken in by inaccurate media images and are prejudiced against those with mental health difficulties, wrongly believing them to be incompetent, unreliable, unpredictable, and dangerous.
For many people, the mass media are their major source of information about mental health. However, the way that problems are portrayed is often unhelpful. Unfortunately frightening stories about unusual events have more ‘news value’. A second reason is the lack of good information available to journalists. In the absence of other sources of material, they currently often have to rely on court cases and inquiries. Obviously this will lead to a preponderance of stories about crime and tragedy. Alternative sources of material are badly needed, as is training for journalists.
We hope that this report will prove to be part of an ongoing major shift in public attitudes that sees prejudice against people with mental health problems become as unacceptable as racism or sexism.
Understanding Psychosis and Schizophrenia is published as a free pdf file by the British Psychological Society, Division of Clinical Psychiatry.































































































You must be logged in to post a comment.